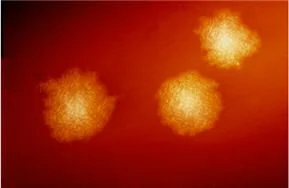
C-Diff is a bacterial infection which causes
3,000 deaths a year in Britain. It affects the digestive system, and is
most common in hospital patients treated with antibiotics for other
infections.
The multi-centre study, carried out by researchers at the
University of Leeds, in partnership with colleagues from the University
of Oxford, University College London and St George’s, University of
London, tested more than 12,000 faecal samples from hospital patients to
establish the best method for diagnosing C-Diff.
The study compared the main different ways of diagnosing
C-Diff, including the two ‘gold-standard’ methods: a cytotoxin assay,
which looks for the presence of C-Diff toxin in faecal samples; and
cytotoxigenic culture, which looks to see if there are bugs present in
faecal samples that could possibly produce C-Diff toxin.
The research team found that patients with faecal samples
positive by the cytotoxin assay were almost twice as likely to die
within 30 days as those patients with samples only positive by the
alternative ‘gold-standard’ method (16.6% versus 9.7%). The findings
mean that tests which detect the presence of toxin in faecal samples
(the cytotoxin assay) are the most reliable indicators of true C-Diff.
Professor Mark Wilcox, of the University of Leeds and Leeds
Teaching Hospitals NHS Trust, who is also the C-Diff lead for Public
Health England, the nation’s public health body, said:
“The diagnosis of C-Diff has become a complicated area with
lots of alternative tests, and there has been considerable uncertainty
about which are the best tests to use.
“This is a landmark study not only because of its size, but
also because we followed what happened to patients. This meant we have
been able to show confidently which are the best tests to use to
diagnose C-diff.
“C-diff cases in the NHS have decreased markedly in number since
their peak in 2007-08 but reliably diagnosing C-diff is a crucial way
forward to continuing to fight this infection.”
These findings highlight the importance of using appropriate
tests to diagnose C-Diff, especially as it is not possible to diagnose
the infection using laboratory tests. Treating patients for C-diff and
preventing the spread of infections in hospitals rely on accurately
identifying who has the infection, but also who may be capable of
transmitting the bug. The study identified a way of using a combination
of tests to identify who has C-diff and who could be at risk of
spreading the bug to others.
The research has already been used as a basis for new 2012 guidelines to the NHS on the diagnosis of C-Diff.
The study was carried out at four hospital sites between October 2010 and September 2011: Leeds Teaching Hospitals NHS Trust, St George’s Healthcare NHS Trust, Oxford University Hospitals NHS Trust and University College London Hospitals NHS Foundation Trust.
The study was funded by the Department of Health and the Health Protection Agency, now known as Public Health England.The findings have been published online in the journal Lancet Infectious Diseases.
Source: University of Leeds